Mar 17, 2014 | Knee, Stem Cell Procedures
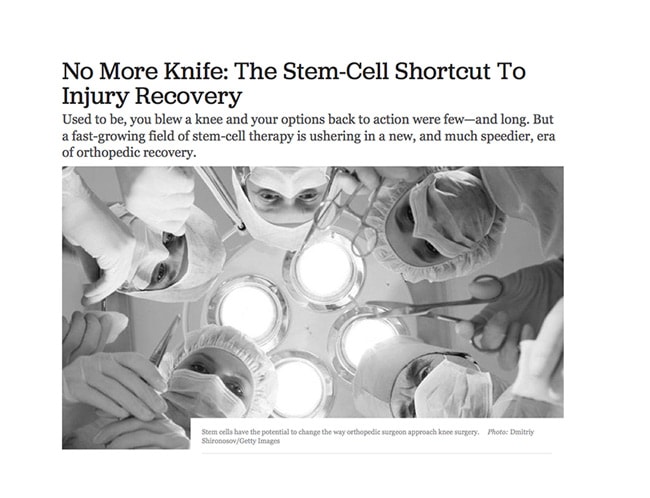
OutsideOnline Magazine just posted a nice article that looks at the Regenexx same-day stem cell procedure for treating ACL tears and the coming wave of biologic treatments that my replace many of the traditional surgeries performed today.
[symple_button color=”blue” url=”http://www.outsideonline.com/fitness/bodywork/the-fit-list/Will-Stem-Cell-Treatments-Replace-Surgery.html” title=”Visit Site” target=”blank” border_radius=””]Read the Article at OutsideOnline[/symple_button]
Jan 21, 2014 | Elbow, Hip, Knee, News and Events, Shoulder / Rotator Cuff, Stem Cell Procedures
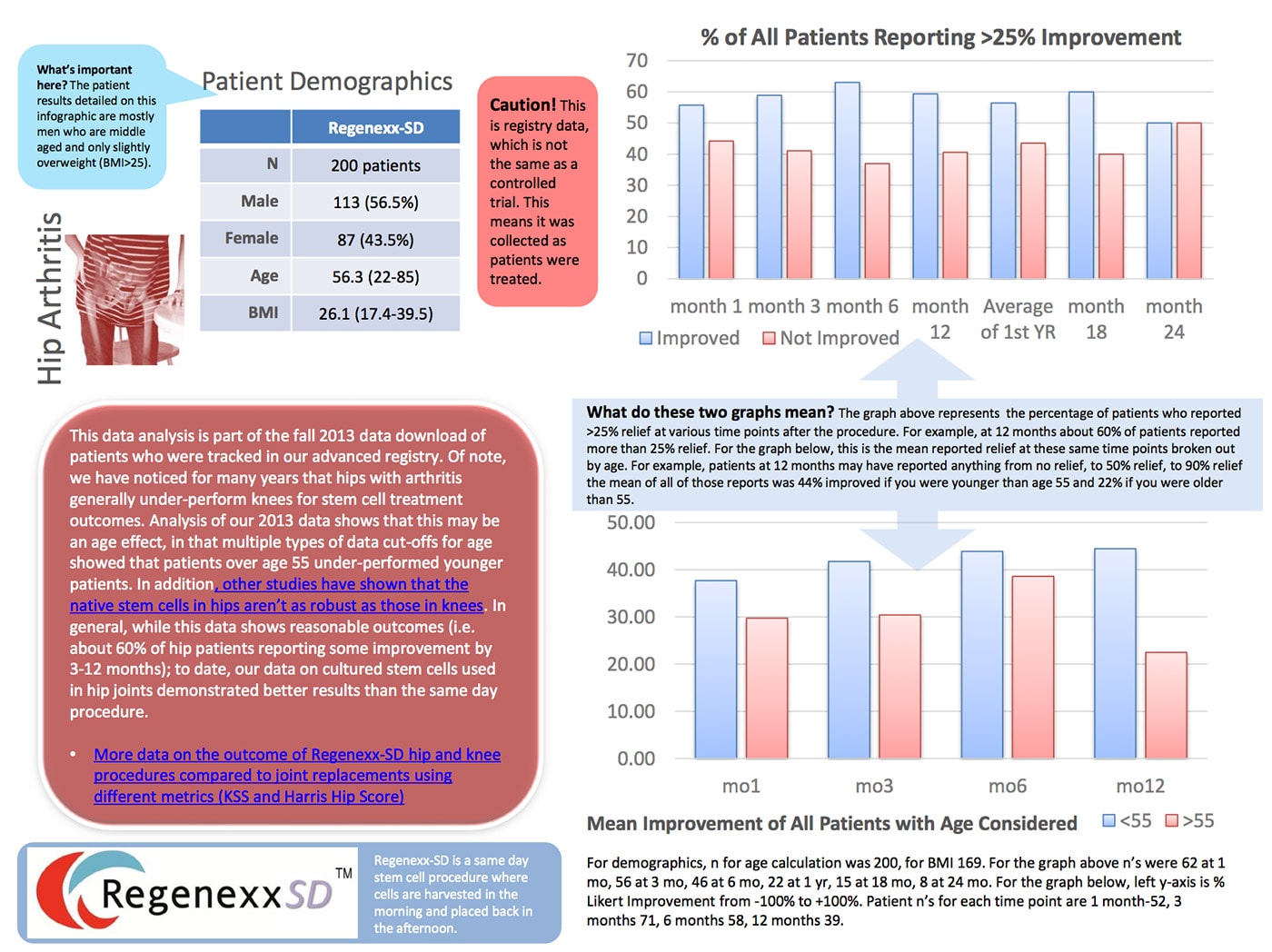
As Regenexx Network Physicians, we’re part of the only stem cell treatment network to publish this type of analysis of patient outcome data. The analysis is made possible thanks to the massive numbers that have been accumulating for years in the Regenexx patient registry.
This patient outcome data is not part of a controlled trial. Every patient becomes part of a registry to track outcomes and any complications. This data is a compilation of patient input to the Regenexx Patient Registry at regular intervals following their Regenexx Procedure.
Jan 21, 2014 | Articles by Body Part, Knee, News and Events, Regenerative Treatments, Stem Cell Procedures
A nice article was recently published at snocountry.com, questioning whether stem cell treatments for the ACL are a “quantum shift” in medicine. Stem cell therapy has shown promising results when compared to traditional surgeries for non-retracted ACL tears and injuries. We are proud to be on the leading edge of these new treatments and articles like these will become more commonplace as athletes become more aware of less invasive alternatives to heal common injuries.
Bob Wislow, 68; Bruce Snyder, 42; and Jacob Gillis, 19, all sought an alternative to surgery that enabled them to regain their high level of activity and remain pain free.
Snyder is a runner, cyclist, and weekend warrior, who tore his meniscus playing soccer. Colorado University student Jacob Gillis, 19, was skiing last spring when he landed awkwardly and heard a “pop” in his knee. An MRI of the ACL (anterior cruciate ligament) showed a partial tear.
Read the complete article at SnoCountry Online
Jan 2, 2014 | Knee, Platelet Lysate, Prolotherapy, PRP, Stem Cell Procedures
Pain Relief through Superior Technology
At StemCell ARTS, we often see patients who have had problems associated with knee surgery, such as a torn meniscus needing repair, surgery to correct an ACL injury or a procedure associated with osteoarthritis. Many of these patients did not experience the results they were hoping for and feel that the surgery has failed. In many cases, the surgery actually did not fail; it just did not go far enough into resolving all of the problems that the patient’s knee joint was experiencing.
Take the example of a torn meniscus surgery. The surgery may have been successful in removing the piece of meniscus that was torn, but it did nothing to address the additional instability in the knee, cartilage wear, or potential tendonitis that the patient might have. These types of issues can cause just as much knee pain as what the patient was experiencing from the initial injury.
Video: Treating Failed Knee Surgeries:
[youtube id=”AjlF-T8VZ0s” width=”600″ height=”350″]
How We Find Additional Knee Issues
The physicians at StemCell ARTS can help diagnose additional knee issues that might still exist after surgery. To confirm the existence of further knee injuries, a local anesthetic or nerve block can be administered to accurately pinpoint whether a certain area is the source of the pain. If pain is relieved, it contributes toward confirming the initial diagnosis. The final diagnosis is confirmed through a review of patient history, a physical examination and other innovative diagnostic procedures. Once diagnosed, a treatment plan, utilizing part or all of the following, can be developed to promote healing.
Stem Cell Therapy: The Process
Stem Cell therapy can be used to help complete the final stages of healing within a knee injury. Stem Cell Therapy makes use of the supply of stem cells available in the body to help repair injured and degenerated tissues. The easiest place to harvest these stem cells is from the back of the hip area, under ultrasound or x-ray guidance. This harvesting procedure is well-tolerated by patients and not considered difficult as many patients claim it is not painful.
After bone marrow blood is drawn, it is centrifuged to concentrate and purify the stem cells, as each stem cell specimen is custom designed to meet the needs of the specific injury. Utilizing either fluoroscopy or ultrasound, the stem cells are precisely injected into the injured site to improve the likelihood that stem cells will adhere to the damaged area and promote healing. After the stem cells are placed, concentrated platelets and other adjuvants are injected to stimulate the stem cells to multiply, and then transform into the repair cells needed to regenerate new cartilage. The platelets are injected again two to five days later to keep the stem cells activated and promote additional healing.
Platelet Rich Plasma
Platelets initiate tissue repair by releasing growth factors. These growth factors start the healing process by attracting cells that repair injuries, including critical stem cells. At StemCell ARTS, our Platelet Rich Plasma Therapy (PRP) intensifies this process by delivering a higher concentration of platelets. The therapy involves a small sample of the patient’s blood, placed in a centrifuge to separate the platelets from the other blood components. The concentrated PRP is then injected into problem areas such as weakened ligaments, injured joints or poor muscle attachments, thus significantly strengthening the body’s natural healing tendencies. StemCell ARTS process for PRP is much different and sets us apart from all others. Because our samples are all hand-processed, we are able to produce PRP that is free of contaminating red and white cells, which can inhibit repair. This same special process also allows us to customize the concentration and volume for each individual and each injury type. This greatly improves patient outcomes. Sometimes just a single injection of PRP will help the knee go through the final stages of repair.
Platelet Lysates
Platelets in the blood release tissue growth factors that aid in the healing process. Normally this occurs slowly over time, but a Platelet Lysate solution that is high in concentration of growth factors can be released immediately into the body. The result is a targeted, faster healing process.
Prolotherapy
Injected three to five days before the stem cells, Prolotherapy contains a solution of concentrated dextrose and a local anesthetic (steroids are not used). This Prolotherapy solution stimulates the body’s natural ability to repair damaged tissue, encouraging new growth and creating a positive environment into which the stem cells are placed.
By introducing additional growth factors, the hidden knee damage that might be present after a failed surgery can finally be encouraged to heal. These treatments can be the key to finally relieving knee pain in a way that marks a real transformation in the patient’s level of mobility and a return to normal life.
Jan 2, 2014 | Knee, Prolotherapy, PRP, Stem Cell Procedures
A recent clinical study found that Regenerative Injection Therapy (RIT) delivered significant improvement in knee function and pain to those suffering from knee osteoarthritis. The study found that study participants receiving RIT treatment experienced an 29.5% improvement in knee pain, stiffness and function measured according to the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC score).[1]
This treatment is just one of many new options available in the fight against knee osteoarthritis. Osteoarthritis of the knee usually occurs in knees that have experienced trauma, infection, or injury. The articular cartilage, which acts as a protective cushion, begins to deteriorate. What these new biological treatments accomplish is assisting and stimulating the growth of new cartilage. It’s an approach that does not simply mask the symptoms, but addresses the root cause of the condition.
[youtube id=”4ZcfslvNPJA” width=”600″ height=”350″]
To maximize healing, Stem Cell treatments are used with other leading treatments in the field including Prolotherapy, Platelet Rich Plasma (PRP) and Platelet Lysate therapy. In certain cases, a patient’s unique medical condition or circumstance may preclude utilizing the benefits of all treatments used together. In this case, a customized plan is developed using one or more of the treatments to obtain the best patient outcomes possible. While sometimes there is no good alternative to surgical repair, most often biologic repair offers a better option.
Stem Cell Therapy: The Process
Stem Cell Therapy makes use of the supply of stem cells available in the body to help repair injured and degenerated tissues. The easiest place to harvest these stem cells is from the back of the hip area, under ultrasound or x-ray guidance. This harvesting procedure is well tolerated by patients and not considered difficult as many patients claim it is not painful.
After bone marrow blood is drawn, it is centrifuged to concentrate and purify the stem cells, with each stem cell specimen custom designed to meet the needs of the specific injury. Utilizing either fluoroscopy or ultrasound, the stem cells are placed on the injured site precisely to improve the likelihood that stem cells will adhere to the damaged area and promote healing. After the stem cells are placed, concentrated platelets and other adjuvants are injected to stimulate the stem cells to multiply, and then transform into the repair cells needed to regenerate new cartilage. The platelets are injected again 2-5 days later to keep the stem cells activated and promote additional healing.
Prolotherapy
With Prolotherapy, a solution of concentrated dextrose and local anesthetic (steroids are not used) stimulates the body’s natural ability to repair the cartilage, encouraging new growth and creating a positive environment into which the stem cells are placed. Prolotherapy treatments are usually scheduled every two to six weeks until the cartilage is regenerated.
Platelet Rich Plasma
Platelets initiate tissue repair by releasing growth factors. These growth factors start the healing process by attracting cells that repair us including critical stem cells. Platelet Rich Plasma therapy intensifies this process by delivering a higher concentration of platelets. The therapy involves a small sample of the patient’s blood placed in a centrifuge to separate the platelets from the other blood components. The concentrated PRP is then injected into and around the point of injury, significantly strengthening the body’s natural healing. Our process for PRP is much different and sets us apart. Because our samples are all hand processed, we are able to produce PRP that is free of contaminating red and white cells, which can inhibit repair. This same special process also allows us to customize the concentration and volume for each individual and each injury type. This greatly improves outcomes.
Platelet Lysates
Platelets in the blood release powerful tissue growth factors that aid in the healing process. Normally this occurs slowly over time, but through the creation of a Platelet Lysate solution, a high concentration of growth factors can be released immediately into the body. The result is a targeted, faster healing process. Additionally, there are areas of the body where using traditional PRP may cause too much inflammation. Platelet Lysates are a better option where inflammation may become an issue.
A Real Solution to Regain Knee Function
These regenerative treatments are a promising revolution in the treatment of knee osteoarthritis. While not a “cure,” these treatments can slow the progression of the disease, significantly reduce pain and restore knee function and mobility to the patient. When combined with short term knee bracing and physical therapy, the effects of this approach can be greatly magnified even further to restore quality of life to most patients.
[1] Richard Dumais, MD, Catherine Benoit, MD, Alex Dumais, MD, Lise Babin, MD, Rachel Bordage, BScN, Claire de Arcos, BScPT, Jacques Allard, PhD, Mathieu Bélanger, PhD, “Effect of Regenerative Injection Therapy on Function and Pain in Patients with Knee Osteoarthritis: A Randomized Crossover Study,” Pain Medicine 2012; 13; 990-999; Wiley Periodicals, Inc.

Jan 2, 2014 | Knee, Prolotherapy, PRP, Stem Cell Procedures
According to a study published in the American Journal of Sports Medicine, out of 295 knee surgeries for Meniscus repair that occurred over a 9-year period, 37 needed subsequent surgeries to correct a failed repair. After a review of medical literature, the study found that the failure rate for this type of surgery could range anywhere from 5-45%[1].
One of the problems with this type of surgery is that when trying to repair these tears, surgeons are often removing Meniscus tissue surrounding the tear. The reason is if the location of the Meniscus tear is on the interior of the knee, the lack of proximity to a blood supply means that the tear may not heal properly. This approach unfortunately can lead to complications including increased arthritis in the knee in the future.
The Meniscus is living tissue acting as a shock absorber in the knee, which is why biologic regenerative treatments hold such promise to actually heal the injury instead of attempting to carve it out. The result is a less invasive procedure, with a quicker return to normal daily activity when compared to surgery. To maximize healing, Stem Cell treatments are used with other leading treatments in the field including Prolotherapy, Platelet Rich Plasma (PRP) and Platelet Lysate therapy. In certain cases, a patient’s unique medical condition or circumstance may preclude utilizing the benefits of all treatments used together. In this case, a customized plan is developed using one or more of the treatments to obtain the best patient outcomes possible. While sometimes there is no good alternative to surgical repair, most often biologic repair offers a better option.
Stem Cell Therapy
Stem Cell therapy makes use of the supply of stem cells available in the body to help repair injured and degenerated tissues. The easiest place to harvest these stem cells is from the back of the hip area, under ultrasound or x-ray guidance. This harvesting procedure is well tolerated by patients and not considered difficult as many patients claim it is not painful.
After bone marrow blood is drawn, it is centrifuged to concentrate and purify the stem cells, with each stem cell specimen custom designed to meet the needs of the specific injury. Utilizing either fluoroscopy or ultrasound, the stem cells are placed on the injured site precisely to improve the likelihood that stem cells will adhere to the damaged area and promote healing. After the stem cells are placed, concentrated platelets and other adjuvants are injected to stimulate the stem cells to multiply, and then transform into the repair cells needed to regenerate new tissue. The platelets are injected again 2-5 days later to keep the stem cells activated and promote additional healing.
Prolotherapy
Injected 2-5 days before the stem cells, Prolotherapy contains a solution of concentrated dextrose and local anesthetic (steroids are not used). This solution stimulates the body’s natural ability to repair damaged tissue, encouraging new growth and creating a positive environment into which the stem cells are placed.
Platelet Rich Plasma
Platelets initiate tissue repair by releasing growth factors. These growth factors start the healing process by attracting cells that repair us including the critical stem cells. Platelet Rich Plasma therapy intensifies this process by delivering a higher concentration of platelets. The therapy involves a small sample of the patient’s blood placed in a centrifuge to separate the platelets from the other blood components. The concentrated PRP is then injected into and around the point of injury, significantly strengthening the body’s natural healing. Our process for PRP is much different and sets us apart. Because our samples are all hand processed, we are able to produce PRP that is free of contaminating red and white cells, which can inhibit repair. This same special process also allows us to customize the concentration and volume for each individual and each injury type. This greatly improves outcomes.
Platelet Lysates
Platelets in the blood release powerful tissue growth factors that aid in the healing process. Normally this occurs slowly over time, but through the creation of a Platelet Lysate solution, a high concentration of growth factors can be released immediately into the body. The result is a targeted, faster healing process. Additionally, there are areas of the body where using traditional PRP may cause too much inflammation. Platelet Lysates are a better option where inflammation may become an issue.
Eliminate the Risks of Surgery
Another recent study demonstrated that a group of patients receiving stem cell treatment experienced double the pain relief compared to a control group in the study over a 2 year period. In particular, one physician from the Mayo clinic monitoring the study noted that there were no adverse events related to the treatment[2]. That fact alone makes biologic regenerative treatments a very attractive option to patients dealing with a Knee Meniscus tear.
[1] Nicolas Pujol, MD, Olivier Barbier, MD, Philippe Boisrenoult, MD and Philippe Beaufils, MD, “Amount of Meniscal Resection After Failed Meniscal Repair,” The American Journal of Sports Medicine; August 2011; vol. 39 no. 8; http://ajs.sagepub.com/content/39/8/1648.abstract
[2] John Gever, Senior Editor, MedPage Today, Reviewed by Zalman S. Agus, MD, Emeritus Professor
University of Pennsylvania School of Medicine and Dorothy Caputo, MA, RN, BC-ADM, CDE, Nurse Planner “Stem Cells Show Promise for Meniscal Tears,” MedPage Today; Feb 10, 2012; http://www.medpagetoday.com/MeetingCoverage/AAOS/31131



