
Jul 6, 2017 | Articles by Body Part, Knee, Prolotherapy, PRP, Stem Cell Procedures
Here at StemCell ARTS, we have seen a recent trend with younger and younger patients. These are intense athletes with aspirations of playing in college and hopefully professionally. Injuries and orthopedic surgeries at an age where children are still developing, puts them at a higher risk for the development of juvenile arthritis. Symptoms manifest much like arthritis in adults, where there is characteristic swelling redness and pain in their joints. Each year, more than 300,000 children are diagnosed with juvenile arthritis. Although there is not yet a cure for it, we are able to provide them with non-surgical solutions to their injuries to help avoid surgery and slow the onset of arthritis.
Common Injuries
The most common problems we see are ACL injuries. These can occur during running, impact and quick changes in direction, most commonly found in sports such as basketball, soccer, and lacrosse. Often, common strains and sprains are able to be treated with Prolotherapy or Platelet Rich Plasma injections. However, for those with more extensive injuries such as tears, we have stem cells to help them heal and get back into the game and their aspirations sooner!
Watch Dr. Newton explain how even a slight injury can end someone’s career for the season, and how we can help avoid that!

Apr 13, 2017 | Blog, Knee, Platelet Lysate, Prolotherapy, PRP, Shoulder / Rotator Cuff, Staff Articles, Stem Cell Procedures
Stem cell and platelet treatments are currently in the spotlight due to their high popularity within the professional sports community. And what’s not to love about them?! Regenerative therapies are minimally invasive, and the recovery and down time is minimal when compared to surgical procedures. These athletes depend on their ability to train hard, and an injury or long recovery is detrimental to their careers. Regenerative procedures give them the option of forgoing more invasive orthopedic procedures (if possible). For example, a standard ACL surgery could have a recovery time of up to six months with the need for rehab, six months of bracing and physical therapy in between. After this surgery, there are also higher chances of early onset arthritis in the knee.
With the procedures offered here at Stem Cell ARTS, we are able to provide athletes with platelet and stem cell injections that will help the body heal itself, with little to no down time! A recovery from our stem cell procedure would require a patient to be non-weight bearing for 48 hours after the stem cells are injected into a weight bearing joint. A brace might be required if deemed necessary by the physician and worn for up to 4 months afterwards. Patients are usually able to go back to the gym for low impact exercises just two weeks post stem cell series. We ask that our patients follow up in six weeks, and typically they are back to their normal physical activities by then!
Who’s Getting Our Procedures?
We are seeing patients of all different ages, backgrounds, and activity levels here in our clinics. More and more young, high school-aged athletes are coming to us after their sports injuries. They are hoping to continue their athletic careers into college and hopefully professionally as well. Years ago, a torn meniscus or ACL would automatically require surgery and, at their young age, there is a higher risk of re-injury. The popularity of CrossFit has (unfortunately) helped us expand our patient base. The intensity of exercise craze has created many common problems such as torn labrums and rotator cuff tendinitis. There has also been an influx of elderly active patients that want to keep their active lifestyles. We have seen patients as young as 90 who have gone back to running marathons after just a few treatments!
The Future of Sports Injuries
It would be an ambitious statement to say that one day, regenerative treatments will replace surgical procedures, but our goal is to help as many people avoid surgery as possible. We are aware that surgery means downtime, and we want to spread the word that there are alternatives out there for you if you want to get back outside in this beautiful weather just in time for spring sports!
Read Dr. Christopher Centeno’s post regarding all the amazing athletes they have treated at our headquarters in Broomfield, Colorado!

Jul 7, 2016 | Knee, Procedure Outcomes, Regenerative Treatments, Stem Cell Procedures
An ACL tear, sustained during a high school lacrosse game, threatened to derail Kellyn Kusyk’s career aspirations of continuing her sport, competitively, at Yale University. Kellyn’s mother, Dr. Casey Kerrigan, specializes in Physical Medicine and Rehabilitation. Dr. Kerrigan was aware of the risks associated with ACL repair surgeries and wanted to avoid surgical intervention, if possible. She knew that it is difficult to completely repair the ACL back to its original integrity. Another major drawback was the downtime and rehabilitation that would follow surgery. Following Kellyn’s consult with StemCell ARTS, she began her first stem cell series of injections to treat her left knee ACL tear. Both Kellyn and Dr. Casey Kerrigan were so impressed with the successful results of Kellyn’s Stem Cell Therapy, they returned approximately 8 weeks later for a second set of injections to ensure that she was in peak condition as she prepared for her career as a collegiate athlete.

May 23, 2016 | Knee, PRP
Regenerative treatments, specifically Platelet Rich Plasma, has been quietly gaining popularity among professional athletes as a way to bounce back quickly after minor injuries such as sprains and strains. Most recently, NBA’s Most Valuable Player, Stephen Curry, has been the newest addition to the growing list of patients receiving platelet procedures. Curry had injured his MCL on April 24th, and was diagnosed with a Grade 1 MCL sprain. These injuries usually occur as a result of twisting or direct impact and can cause tenderness, stiffness, and mild swelling at the injury site.
These injuries would usually be detrimental to an athlete, and continuing to play with an injury could cause further harm. However, Curry received PRP treatment within two days of his injury and was able to return after missing only two games. His Platelet Rich Plasma treatment involved concentrating a blood sample and isolating growth factors to inject back into the injured site in order to promote healing. The procedure is minimally invasive and athletes are able to return to light or normal activity soon afterwards
http://www.foxsports.com/nba/story/stephen-curry-golden-state-warriors-what-is-platelet-rich-plasma-therapy-050416
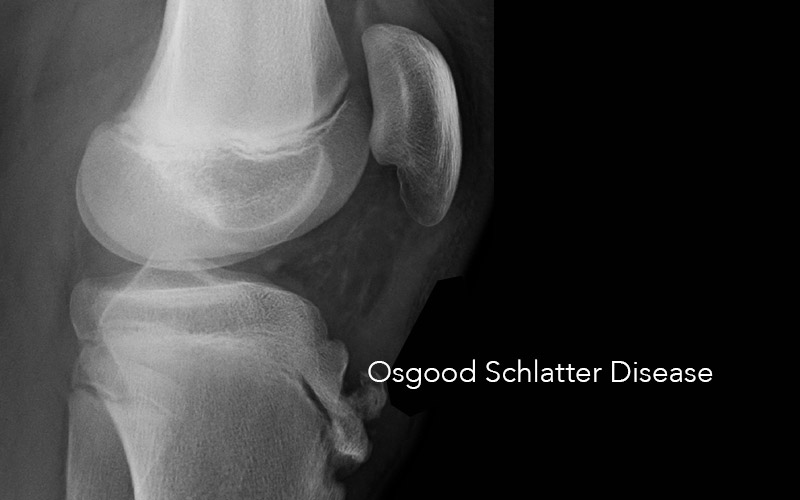
Jun 8, 2015 | Knee, Research
Osgood Schlatter’s Disease (OSD) is very common in young adolescents, affecting millions of young people a year, and represents damage to the tendon to cartilage connection on the bony prominence just below the knee cap. If it does not respond quickly to sports limitation, it often leads to substantial alteration of sports ability/participation for a year or more, affecting career development, athlete confidence and self-esteem development and peer relationships for the young athlete. It also causes chronic pain and sports limitations even in adulthood in a substantial number of athletes as well as an obvious deformity. The OSD study that Dr. Reeves designed and published in conjunction with primary author Gaston Topol in Argentina was directed toward investigating the potential to cure OSD early, to decrease the above consequences.
View the study here: http://www.aaomed.org/Osgood-Schlatter-Disease

Jan 21, 2015 | Knee, News and Events, Regenerative Treatments, Stem Cell Procedures
On The Snow recently published this excellent article, showing that skiers are increasingly turning to Regenexx Stem Cell procedures to treat ACL injuries.
I entered the room where a Halloween-prop-sized needle was being cored down into the patient’s hip still skeptical that this procedure was “comfortable” and “painless” as I had read. But, after carrying on a conversation with the patient—who was, admittedly, doing much better than I at that moment, chatting calmly about feeling only pressure as the needle filled with blood—I exited the room a believer.
Read the full article at On The Snow.






